The Nail Plate: Structure, Layers, Growth and Clinical Changes
Author: Radina Ignatova, Professional Nail Expert & International Nail Educator | Last Updated: March 2026
Quick Summary
The nail plate is the hard, translucent structure that forms the visible nail. It is produced by the nail matrix and built from three distinct layers — dorsal, intermediate, and ventral — each with a specific job to do.
For nail professionals, understanding the nail plate is not optional background knowledge — it is the foundation of every safe, informed service decision. Its thickness, condition, and layer integrity directly affect how products perform, how long results last, and how much risk a service carries for a particular client.
Contents
- What Is the Nail Plate?
- The Three-Layer Structure
- What the Nail Plate Is Made Of
- Thickness: What Is Normal?
- Growth and Regeneration
- How the Nail Plate Behaves
- What Damages the Nail Plate
- Clinical Changes Professionals Should Recognise
- What This Means in the Salon
- Common Misconceptions
- Frequently Asked Questions
What Is the Nail Plate?
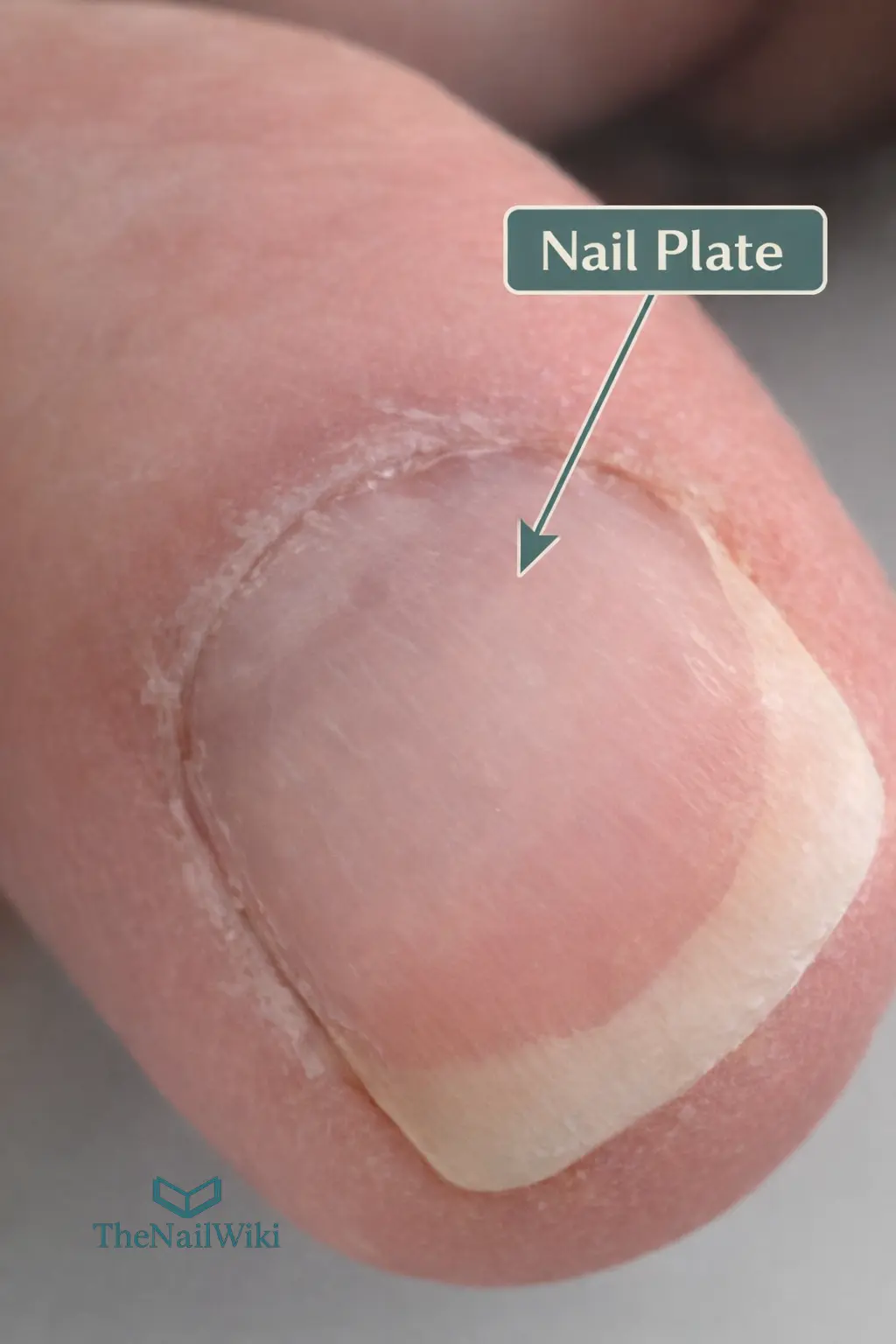
The nail plate is the hard, keratinised structure that sits on top of the fingertip or toe. It runs from beneath the proximal nail fold at the base all the way to the free edge — and everything visible when you look at a nail is the nail plate. It belongs to the same family of structures as hair; both are ectodermal appendages, produced through a process of progressive keratinisation. The key difference is that the nail plate grows as a continuous flat sheet rather than a strand, and it does not go through cycles of shedding the way hair does.
Its job is more functional than most clients realise. The nail plate creates a firm backing surface against which the soft pad of the fingertip presses when gripping, touching, or manipulating objects — this is what makes precision tasks possible. It also protects the bone and soft tissue of the distal phalanx underneath it. Without it, even simple daily tasks become painful and difficult.
From a chemistry standpoint, the nail plate behaves quite differently from skin. Skin relies heavily on a lipid-rich outer barrier; the nail plate has very little lipid content and depends almost entirely on its compacted keratin structure for strength and protection. This is why it responds to water, solvents, and product exposure in ways that skin does not — and why understanding it matters for anyone applying products to it professionally.
The Three-Layer Structure
The nail plate is not a single uniform block of keratin. It is built in three distinct layers — the dorsal layer, the intermediate layer, and the ventral layer — each with its own cellular architecture and its own specific role. Understanding this is directly relevant to salon work, because different types of damage target different layers, and the consequences depend on which layer is affected.
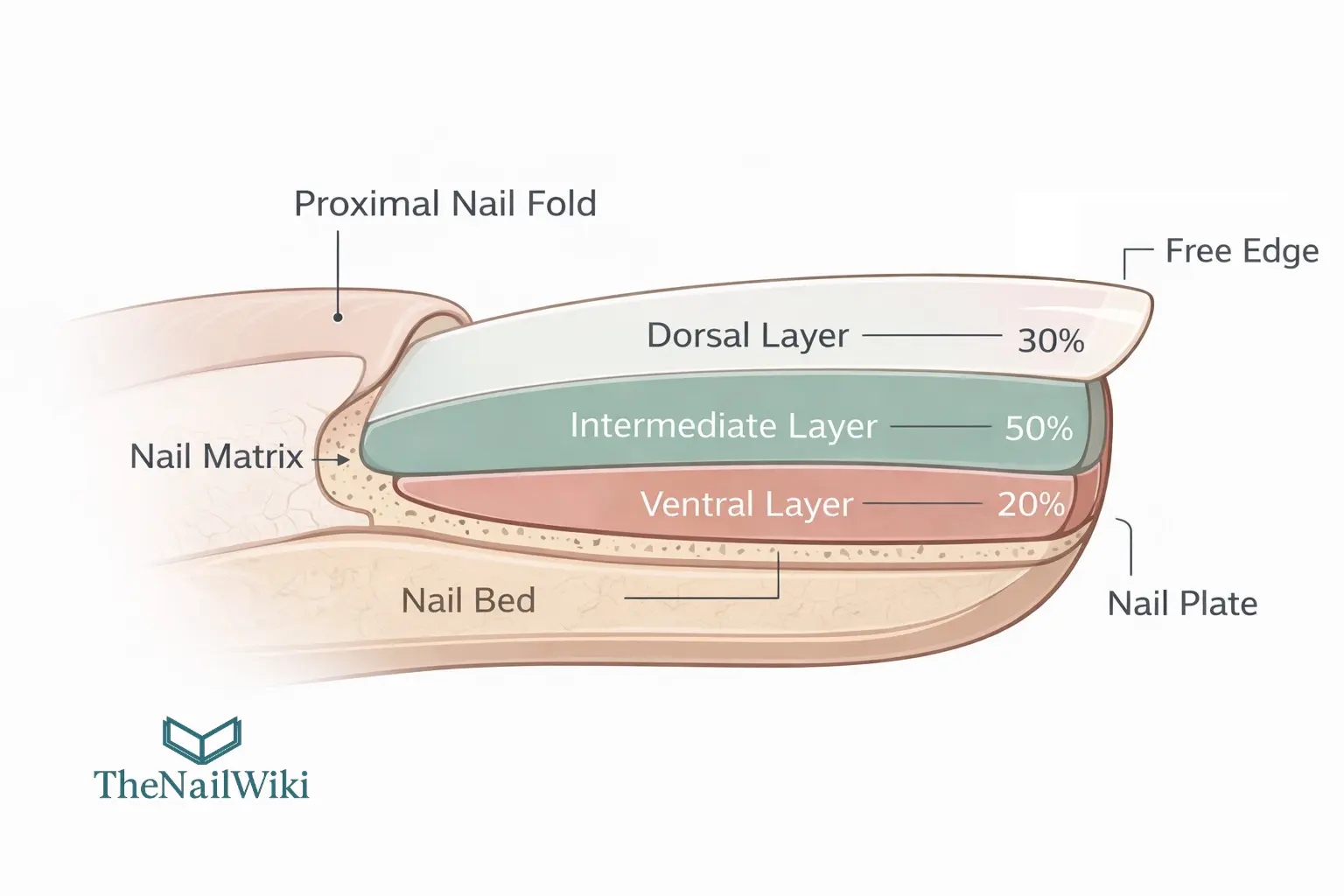
The Dorsal Layer — the outer surface
The dorsal layer is the outermost portion of the nail plate — the surface you see and touch. It accounts for roughly 30% of the total plate thickness and is characterised by comparatively flat, tightly packed cells that give the surface its hardness and smoothness. This is the layer that produces the natural shine of a healthy nail, and it is the first to show the effects of surface disruption. Aggressive filing, buffing, or mechanical trauma from poorly fitted tools all affect the dorsal layer first. Once it is roughened or thinned, the visible change — dullness, surface irregularity, or micro-peeling — is a direct reflection of structural compromise at this level.
The Intermediate Layer — the structural core
The intermediate layer is the thickest of the three, making up approximately 50% of the nail plate’s total depth. Its cells are more strongly interdigitated — meaning they lock together more firmly — which is what gives the plate the bulk of its mechanical strength and resistance to bending forces. Most of what we think of as “nail strength” lives here. Disease processes that originate in the nail matrix — the tissue that produces the plate — feed their output primarily into this layer, which is why conditions affecting the matrix tend to produce visible structural changes that persist for months as the affected section of plate grows forward.
The Ventral Layer — the attachment interface
The ventral layer is the thinnest of the three, accounting for approximately 20% of total thickness. It sits directly above the nail bed and its undersurface is deliberately irregular — this roughness supports the physical interlock between the nail plate and the nail bed beneath it. It is produced by the distal matrix (also referred to in some literature as the sterile matrix), and notably may be absent or significantly reduced in the region above the lunula, meaning that the proximal portion of the nail plate is essentially a two-layer structure in some individuals. Changes affecting the ventral surface are directly relevant to onycholysis — the separation of the plate from the nail bed — as the integrity of this layer is central to maintaining that attachment.
| Layer | Proportion | Primary role | What damage looks like |
|---|---|---|---|
| Dorsal | ~30% | Surface hardness, smoothness and natural shine | Dullness, roughness, surface peeling, micro-scratching |
| Intermediate | ~50% | Mechanical strength, toughness and flexibility | Thinning, splitting, structural weakness, visible ridging |
| Ventral | ~20% | Adhesion to the nail bed | Onycholysis — plate lifting away from the nail bed |
Proportions are indicative based on commonly cited ratios in nail biology literature. Actual values vary between individuals.
What the Nail Plate Is Made Of
The nail plate is built almost entirely from onychocytes — fully keratinised cells that have completed their life cycle within the nail matrix. By the time they become part of the finished plate, these cells have lost their nucleus and all internal organelles; they are essentially densely packed packets of keratin protein, held together by a network of structural bonds and a thin intercellular cement layer between them.
The keratin in the nail plate is a mixture of two types: hard keratins (the same family found in hair) and epithelial keratins (the type found in skin). The hard keratins are responsible for the plate’s characteristic rigidity and resistance to deformation. These are reinforced by disulfide cross-links — chemical bonds between sulphur-rich proteins — which are what give the nail plate its structural strength. This is the same principle behind the strength of hair; a high sulphur content, densely cross-linked, creates a tough and resilient material.
Between the onychocytes sits a thin intercellular cement — thought to contain structural proteins and polysaccharides — that holds the layers together as a cohesive unit. When this cement is disrupted by repetitive mechanical stress, solvent exposure, or dehydration cycles, the result is often lamellar splitting or peeling at the free edge: the layers begin to separate because the material binding them has been weakened.
Water and Lipid Content
The nail plate contains very little lipid — estimated at around 0.1 to 1% — which is significantly less than the outermost layer of skin. This is an important distinction: it means the nail plate cannot use a lipid barrier the way skin does, and is considerably more permeable to water movement than skin under equivalent conditions.
Water content is variable and environment-dependent. Measured values in published research span a wide range — from under 5% in very dry ambient conditions to over 30% in saturated environments — with typical in-vivo readings in temperate climates generally falling between approximately 7% and 18%. Seasonal variation has been documented, with nails tending to hold less water in winter than in summer. The practical point is that there is no single “normal” water content; it shifts constantly with the environment, the client’s habits, and any products or solvents they have been exposed to.
Why this matters in practice: Because the nail plate’s barrier is keratin-based rather than lipid-based, solvents such as acetone penetrate it more readily than they penetrate skin. Research has shown that repeated acetone exposure can reduce the ceramide fraction within the nail plate and lower its water-holding capacity — contributing over time to the dryness, brittleness, and free-edge peeling that many clients associate with frequent polish removal.
Thickness: What Is Normal?
Nail plate thickness varies considerably between individuals, between digits on the same hand, and even between measurement methods — so there is no single figure that applies universally. For fingernails, the range most commonly cited in biophysical and clinical research falls between approximately 0.25 mm and 0.60 mm, with many published mean values sitting between 0.35 and 0.50 mm. Toenails are substantially thicker, with values reaching approximately 1.3 mm in some populations.
Reference ranges at a glance
- Fingernails: approximately 0.25 – 0.60 mm (mean typically 0.35 – 0.50 mm)
- Toenails: up to approximately 1.3 mm
- Dorsal layer alone: approximately 0.10 – 0.18 mm (illustrative, based on 30% of total)
These are population ranges. Individual thickness will vary and is affected by age, health status, nutrition, and prior service history.
What makes these figures clinically significant for nail professionals is the relationship between thickness and vulnerability. A plate at the lower end of the normal range — say 0.25 to 0.30 mm — has very little margin before it becomes mechanically compromised. Research documenting average thickness reductions of approximately 0.04 mm per cosmetic service cycle involving surface abrasion shows that this loss is real and measurable. Across eight or ten appointments, a thin plate can lose a meaningful proportion of its total depth — and the effect is cumulative.
Growth and Regeneration
Where the Nail Plate Comes From
The nail plate is produced entirely by the nail matrix — the specialised tissue located beneath the proximal nail fold at the base of the nail. Matrix keratinocytes divide, migrate distally, and progressively keratinise until they form the compacted onychocytes of the finished plate. Different parts of the matrix contribute to different layers: the proximal matrix generates the dorsal and intermediate layers, whilst the distal matrix contributes to the ventral layer and helps anchor the plate to the nail bed below.
This regional contribution has important clinical implications. Because the proximal matrix produces the majority of plate volume, damage to this area carries the greatest risk of permanent deformity. Significant scarring within the proximal matrix — from trauma, aggressive filing into the base area, surgical procedures, or progressive inflammatory disease — can result in persistent ridging, thinning, or in severe cases, failure of the plate to regrow at all. This is one of the reasons that any service involving significant mechanical work near the matrix zone warrants particular care.
How Fast Nails Grow
Fingernails grow at an average of approximately 3 to 3.5 mm per month under normal conditions. Toenails grow at roughly one third to one half that rate — approximately 1.5 to 1.6 mm per month. Complete regrowth of a fingernail from base to free edge takes approximately six months; a toenail takes twelve to eighteen months. These timelines matter practically when a client is recovering from nail damage or managing an ongoing nail condition — setting realistic expectations is far easier when these figures are familiar.
Growth is not equal across all fingers. The thumbnail and middle finger typically grow the fastest; the little finger grows the most slowly. Growth also declines with age — this is well established in the research literature. Long-term observations tracking individual growth rates document reductions of 20–25% or more between early adulthood and older age. For older clients, this slower turnover means that any damage takes proportionally longer to grow out, and recovery from trauma or product-related thinning is a lengthier process than it would be for a younger client.
What Slows Growth
Several systemic factors are known to reduce nail growth rate. These include significant illness, nutritional deficiency (particularly low protein intake), physical immobilisation of the digit or limb, compromised immune function, and certain medications — particularly anti-mitotic drugs used in oncology. When growth slows significantly, the plate produced during that period may be structurally weaker or thinner than usual, sometimes manifesting later as a visible transverse groove (Beau’s line) once normal growth resumes. Recognising this pattern helps professionals contextualise sudden changes in nail plate quality and communicate effectively with clients about what they are seeing.
How the Nail Plate Behaves
Hardness, Flexibility and Curvature
The nail plate is hard relative to soft tissue but retains a degree of flexibility — and that flexibility increases significantly with hydration. A dry nail plate is stiffer and more prone to cracking or snapping under bending load; a well-hydrated plate is more pliable and absorbs force more effectively. This relationship between water content and mechanical behaviour is one reason why prolonged soaking before nail services can be counterproductive — it temporarily increases flexibility to the point that the plate is more susceptible to distortion, and it takes time to return to a stable state afterwards.
The natural curvature of the nail plate — both lengthways (longitudinal arch) and across the width (transverse arch) — is mechanically important. This double curve distributes applied forces across the plate surface and makes the structure more resistant to bending at any single point. When a nail becomes significantly thinned in a localised area, this load-distribution advantage is reduced and the plate is more likely to crack, split, or lift at that site. It also explains why structurally compromised nails often fail at the same point repeatedly until the underlying thinning resolves.
It is worth noting that a thicker nail plate is not automatically a stronger one. Research examining nails affected by onychomycosis found that infected plates — which were nearly twice the thickness of healthy nails — had tensile strength roughly one third lower than unaffected plates. The quality and integrity of the keratin architecture matters as much as the raw measurement of depth.
What Damages the Nail Plate
Filing and Abrasion
Surface abrasion does more than remove material from the top of the plate. Research measuring trans-onychial water loss — the rate at which water passes through the nail plate — has demonstrated that filing the surface significantly increases this rate, and the effect does not immediately resolve once the abrasion stops. This indicates that surface disruption alters the plate’s barrier behaviour at a structural level rather than simply creating a smoother or rougher surface. The more aggressive the abrasion, and the more frequently it is repeated, the greater the cumulative impact on how the plate manages moisture and its overall structural integrity.
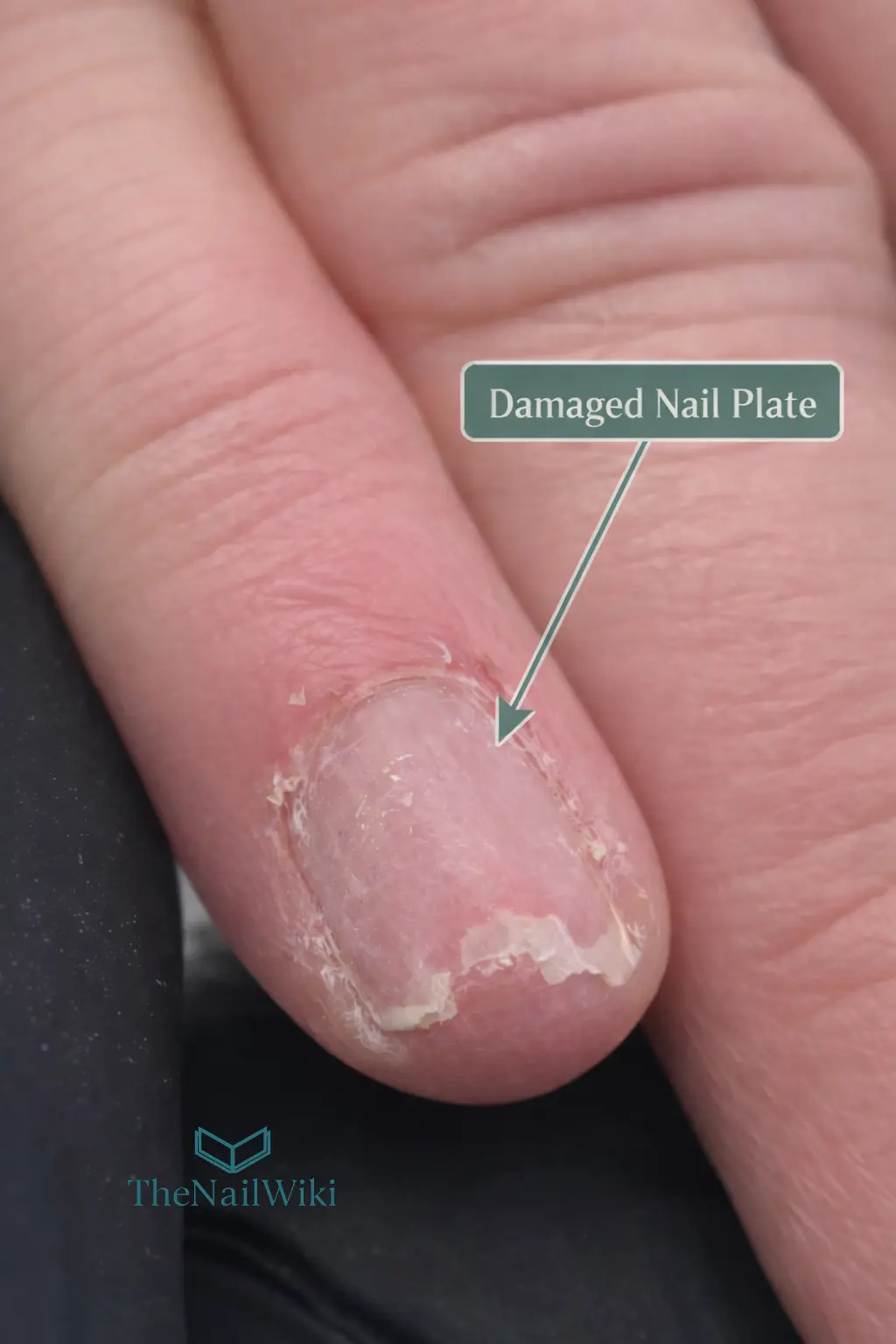
The professional standard: Apply only the abrasion necessary for the service being performed. The nail plate has no capacity to repair itself — the damaged section must grow out and be replaced. For a client already presenting with thin or compromised nails, even a single over-zealous preparation pass can set recovery back significantly. The client photographed above required approximately eight months of consistent manicure appointments, cuticle care, and conditioning treatment before the nail plate returned to near-healthy condition.
Over-Filing, Layer Exposure and the Risk of Sensitisation
There is a consequence of over-filing that goes beyond structural damage — and it is one that every nail professional needs to understand clearly. When aggressive abrasion removes the dorsal layer and begins to compromise the intermediate layer, the nail plate becomes significantly thinner and more permeable. At this point, any product applied to the nail surface — gel, acrylic, builder gel, bonding agent — is no longer sitting on an intact, resilient structure. It is in direct or near-direct contact with tissue that is far closer to the living nail bed than it was designed to be.
This matters because the chemicals in nail products — including monomers, photoinitiators, and adhesion promoters — are formulated on the assumption that the nail plate is providing a meaningful physical barrier between the product and the living tissue beneath. When that barrier has been thinned to the intermediate or ventral layer, the distance between product chemistry and the nail bed is dramatically reduced. The result is increased chemical penetration into the periungual tissues, and with it, an elevated risk of contact sensitisation.
Why this is a sensitisation risk, not just a comfort issue
Contact sensitisation occurs when the immune system is exposed to a chemical in sufficient quantity to register it as a threat. Once sensitised, a client may develop a reaction to that chemical — or to related chemicals in the same family — on every subsequent exposure, for life. There is no desensitisation process. The reaction typically worsens with repeated contact rather than improving.
Over-filed nails increase the risk of this occurring because they remove the physical barrier that keeps product chemistry at a safe distance from living tissue. A client who has had their nails repeatedly over-filed is not just a client with thin nails — they are a client at elevated risk of developing a permanent allergy to nail products.
Product retention is also directly affected. When the dorsal layer has been removed and products are applied to a compromised intermediate or ventral layer, adhesion quality deteriorates — the surface energy, texture, and structural stability of the underlying layer are not equivalent to those of an intact dorsal surface. Clients and technicians sometimes interpret this as a product failure or a formulation issue; in many cases, it is a preparation issue rooted in over-abrasion of the nail plate.
The correct response when encountering a significantly thinned plate is not to press ahead with a standard service. It is to assess whether proceeding is appropriate, adjust the preparation protocol accordingly, and in cases of severe compromise, advise the client that the nail plate needs to recover before further enhancement services can be safely applied.
Solvent Exposure
Acetone-based nail polish removers are effective and widely used — but their repeated application has measurable consequences for nail plate structure. Experimental research has found that acetone exposure reduces the ceramide fraction within the plate, lowers water-holding capacity, and produces morphological changes at the distal free edge including surface roughness and lamellar peeling. The nail plate cannot replenish its lipid content between exposures the way skin can, which is why the effects accumulate more readily with frequent use.
This does not mean acetone should be avoided entirely — it remains the most effective solvent for product removal in many systems. It does mean that unnecessary soaking time should be minimised, that clients with already fragile or thin plates may benefit from added support between services, and that awareness of these effects should inform how removal processes are carried out.
Repeated Wetting and Drying
Repeated cycles of wetting and drying are among the most common — and underestimated — contributors to nail plate fragility. Each wetting event temporarily swells the plate; each drying event causes it to contract. Over time, this mechanical stress degrades intercellular adhesion, particularly at the free edge where the plate is unsupported beneath, leading to the lamellar splitting and distal peeling that professionals see frequently in clients who work with their hands in water or who are frequent hand-washers. This is not a product failure — it is a structural consequence of environmental exposure, and managing it requires an understanding of the underlying biology.
Clinical Changes Professionals Should Recognise
Important: The following information is educational. Many nail plate changes share a similar appearance, and a visual assessment alone is never sufficient for diagnosis. Any change that is painful, rapidly progressing, affects multiple nails, or does not resolve within a reasonable timeframe should be assessed by a medical professional. Nail professionals are not diagnosticians — but they are often the first to notice that something needs further investigation.
Onycholysis — when the plate lifts from the nail bed
Onycholysis is the separation of the nail plate from the nail bed beneath it. It typically begins at the distal or lateral edge and produces a white or opaque area, because air filling the gap changes the way light passes through the plate. The separated section is usually painless but creates a pocket where moisture and microorganisms can accumulate. Causes range from mechanical trauma — including repetitive stress from tight footwear or overly aggressive filing at the free edge — to inflammatory skin conditions, fungal infection, systemic disease, and certain medications. A dedicated page covering onycholysis in full is available in the Nail Wiki Library — Onycholysis.
Pitting — surface depressions in the plate
Nail pitting refers to small punctate depressions on the dorsal surface of the plate. They form when a localised area of the nail matrix produces cells that are poorly formed or shed prematurely, leaving a visible indentation in the surface as that section of plate grows forward. Pitting is most strongly associated with psoriasis and alopecia areata. In psoriasis, pits tend to be deeper, wider, and randomly distributed; in alopecia areata, they are typically shallower, smaller, and may appear in a more regular pattern. Neither presentation should be treated without medical assessment. Full detail is covered in the dedicated Nail Pitting library page.
Beau’s Lines — transverse grooves
Beau’s lines are horizontal grooves that cross the width of the nail plate. They form when the nail matrix experiences a significant but temporary interruption to its normal output — producing a thinner section of plate during the affected period. Once normal growth resumes, this thin band moves distally and becomes visible as a groove. When Beau’s lines appear at a comparable position across several nails simultaneously, they point to a systemic cause — a period of serious illness, physiological stress, or a medication effect. The approximate timing of the causative event can often be estimated from the groove’s current position relative to the proximal nail fold and the average growth rate. Full detail is covered in the dedicated Beau’s Lines library page.
Brittleness and Lamellar Splitting
Brittle nail presentations are common and varied. They include lamellar splitting or peeling at the free edge (onychoschizia), longitudinal fissuring and ridging (onychorrhexis), surface granulation of the dorsal plate, and nails that appear short or worn despite no deliberate cutting. Reported prevalence in the general population is up to approximately 20%, with a higher proportion in women over fifty. Environmental exposures — particularly repeated wetting and drying, detergent contact, and solvent use — are significant contributing factors, as is the cumulative effect of abrasive nail services over time.
What This Means in the Salon
Nail anatomy is not abstract knowledge — every piece of it connects directly to decisions made at the nail desk. Here is how the biology of the nail plate translates into professional practice.
Treat thickness as a non-renewable resource
The nail plate cannot self-repair. Any material removed through abrasion is gone until the plate grows out — which takes months. For clients with naturally thin plates, or those who have experienced previous over-filing, each service should begin with a deliberate assessment of current plate thickness and an adjustment of preparation technique accordingly. Minimum necessary abrasion is not a compromise on the service; it is the correct professional standard.
Surface state determines product performance
The physicochemical state of the nail plate surface at the moment of product application directly influences adhesion quality. A contaminated surface — residual oils, moisturiser, or inadequate dehydration — reduces the surface energy available for bonding. Conversely, a surface that has been over-abraded presents an unstable barrier layer with altered water-handling properties. Optimal surface preparation achieves cleanliness and appropriate surface texture without structural disruption — which requires an understanding of both the product system and the biology of the surface being prepared.
Know when to decline and refer
A nail professional is frequently the first person to observe changes in the nail plate that may indicate an underlying condition — and that is a significant responsibility. Onycholysis of unknown cause, unexplained pitting, rapid structural changes, pigmentation within the plate, or persistent brittleness that does not resolve with appropriate care all warrant a conversation with the client and, in most cases, a referral for medical assessment. Applying nail products over pathological changes does not resolve the underlying issue; it delays assessment and may worsen the outcome.
Structured professional training that addresses nail anatomy in depth — rather than simply product application technique — gives technicians the confidence to identify these situations and respond appropriately. Anatomy-informed courses are available through Artistic Touch Nail Training Academy for professionals who want to practise with a higher level of clinical awareness.
Common Misconceptions
❌ “Nails need to breathe”
The nail plate does not perform gas exchange. It is an inert keratinised structure — it does not breathe, and it has no biological need for air contact. Oxygen reaches the nail bed and matrix through the underlying blood supply, not through the nail surface. This claim has no anatomical basis, and the “nail breaks” it is used to justify are not supported by nail biology.
❌ “Brittle nails just need more moisture”
Clinical research has not found consistently lower water content in brittle nails compared with unaffected ones. Brittleness is multifactorial — it involves intercellular adhesion quality, cumulative exposure history, mechanical microdamage, and individual plate composition. Hydration can support flexibility but cannot correct the structural causes of brittleness on its own.
❌ “A thicker nail is a stronger nail”
Thickness and structural integrity are not the same thing. Research on nails affected by fungal infection found that infected plates — which were nearly twice as thick as healthy nails — had significantly lower tensile strength and stiffness. The quality of the keratin architecture within the plate matters as much as the total depth measurement.
❌ “Filing the surface only removes dead cells”
All cells in the nail plate are keratinised — there is no separate layer of “dead” surface cells to remove in the way there is with skin. Filing the nail plate surface removes structural material from the dorsal layer and disrupts the plate’s barrier properties. This is measurable and cumulative. The rationale for surface abrasion in nail preparation should be product adhesion, not cell removal.
Frequently Asked Questions
What is the nail plate made of?
The nail plate is built from onychocytes — fully keratinised cells produced by the nail matrix. It contains a mixture of hard (hair-type) and epithelial (skin-type) alpha-keratin proteins, reinforced by disulfide cross-links between cysteine-rich structural proteins. Lipid content is very low, and water content varies considerably with environmental conditions and exposure history.
How thick is the average nail plate?
For fingernails, total nail plate thickness is commonly reported within a range of approximately 0.25 to 0.60 mm, with many published mean values between 0.35 and 0.50 mm. Toenails are considerably thicker — up to approximately 1.3 mm in some populations. Thickness varies between digits, sexes, and individuals, and also changes with age and service history.
How long does it take for a nail plate to grow out fully?
A fingernail plate takes approximately six months to grow out completely from base to free edge. Toenails grow at roughly one third to one half the rate of fingernails and typically require twelve to eighteen months for full regrowth. These timelines are the reason nail damage — including product-related thinning — can take so long to fully resolve.
Does filing damage the nail plate permanently?
Filing removes structural material from the dorsal layer and measurably alters the plate’s barrier behaviour — effects that do not immediately resolve. Whether this constitutes “permanent” damage depends on the degree of abrasion and whether it is repeated. A single preparation pass at an appropriate grit causes minimal lasting disruption. Repeated aggressive abrasion over multiple service cycles can produce cumulative thinning that significantly compromises the plate until it grows out completely.
Why does onycholysis cause a white appearance?
Under normal attachment, the close contact between the nail plate and nail bed allows light to pass through in a way that produces the characteristic pink translucency of a healthy nail. When the plate separates and air fills the gap, light scatters differently, producing a white or opaque appearance at the separated area.
What causes Beau’s lines?
Beau’s lines form when nail matrix output is significantly but temporarily reduced, producing a thinner section of plate. Once normal growth resumes, this thinner band moves distally and becomes visible as a horizontal groove. When lines appear at a similar position across multiple nails simultaneously, they typically indicate a systemic event — serious illness, significant physiological stress, or a medication effect — at a calculable point in the past.
Can over-filing cause a nail product allergy?
Yes — and this is one of the most serious risks associated with aggressive over-filing. When the nail plate is thinned to the intermediate or ventral layer, the physical barrier between product chemistry and the living tissue of the nail bed is significantly reduced. Nail product ingredients — including monomers, photoinitiators, and adhesion promoters — can then penetrate closer to living tissue than they should, increasing the risk of contact sensitisation. Once sensitised, a client may react to that chemical family on every future exposure, for life. Over-filing is therefore not just a structural concern — it is a direct sensitisation risk, and it is one of the reasons that minimum necessary preparation is a professional safety standard, not simply a technique preference.
Can the nail plate fully recover after being damaged by over-filing?
Yes — provided the nail matrix has not been injured, the plate will grow out and replace the damaged section over time. Realistically, severe over-filing damage can take six to eight months or longer to resolve fully, even with consistent professional care. The client photographed in Figure 3 on this page required approximately eight months of regular manicure appointments, cuticle conditioning, and supportive care before the nail plate returned to near-healthy condition. There is no way to accelerate this, and no topical product can repair a thinned plate in place. Management focuses on protecting the compromised plate, avoiding all further abrasion, and setting realistic expectations from the outset.
Related Library Pages
Nail Anatomy
- → The Nail Matrix
- → The Nail Bed
- → The Hyponychium
- → The Eponychium and Cuticle
- → The Lunula
- → How Nails Grow
Nail Conditions
- → Onycholysis — Nail Plate Separation
- → Beau’s Lines — Transverse Nail Grooves
- → Nail Pitting
- → Brittle Nails — Onychoschizia and Onychorrhexis
- → Onychomycosis — Fungal Nail Infection
Professional Safety
- → Contact Sensitisation and Nail Allergies
- → Nail Contraindications
- → Patch Testing for Nail Products
- → E-File Safety
Some linked pages are currently in development and will be published progressively. The library is updated regularly.
Professional Disclaimer
The information on this page is provided for educational purposes and is intended to support the professional knowledge of nail technicians and nail educators. It does not constitute medical advice. Any client presenting with nail plate changes that may indicate underlying pathology should be advised to seek assessment from a qualified medical professional. TheNailWiki does not endorse specific products or treatment protocols.
About the Author
Radina Ignatova
Professional Nail Expert since 2014 | International Nail Educator | Founder of TheNailWiki and Artistic Touch Nail Training Academy
Radina Ignatova is a Professional Nail Expert since 2014 and an International Nail Educator specialising in dual forms, gel systems, polygel application, advanced nail structure, E-File techniques and professional salon safety.
She founded TheNailWiki to provide clear, safety-led nail education accessible to everyone, and Artistic Touch Nail Training Academy to deliver structured professional online nail courses.
Her teaching philosophy is centred on honest education — demonstrating real salon challenges, practical corrections and performance-based techniques rather than presenting only polished results.
Based in Scotland, UK, Radina contributes to advancing professional standards within the nail industry through structured educational resources and technical training.
Read full bio →About TheNailWiki
TheNailWiki is an independent educational platform dedicated to providing accurate, safety-led and professionally informed nail care information to professionals and enthusiasts worldwide. All content is created by qualified nail industry professionals and reviewed for technical accuracy.
Our mission is to provide accurate, safety-focused and professionally informed nail education that is accessible to everyone. For structured professional training, advanced masterclasses, and specialist technique courses, visit Artistic Touch Nail Training Academy.
This library page is published by TheNailWiki — an independent nail education resource maintained by nail industry professionals. Content is safety-led and professionally informed. TheNailWiki is editorially independent and does not accept payment to influence library content. For editorial standards, visit thenailwiki.com/editorial-standards/.
