Onycholysis: Causes, Recognition and Professional Management
Author: Radina Ignatova, Professional Nail Expert & International Nail Educator | Last Updated: March 2026
Quick Summary
Onycholysis is the separation of the nail plate from the nail bed beneath it. It is one of the most frequently encountered nail conditions in the professional salon setting and one of the most commonly mishandled. It presents as a white or pale area beginning at or near the free edge and progressing towards the base of the nail.
Once the plate-to-bed attachment breaks, it does not spontaneously repair itself in the separated zone. The only path to recovery is to remove the cause, trim the lifted section back to solid attachment, and allow the nail bed to re-establish its bond with the advancing plate as it grows forward.
Contents
What Is Onycholysis?
Onycholysis is the clinical term for the detachment of the nail plate from the nail bed. Under normal conditions, the nail plate is firmly bonded to the nail bed along its entire length through a continuous epidermal attachment — a biological bond maintained throughout the nail’s growth cycle. When this bond breaks down in any part of the nail, the result is onycholysis.
The word derives from the Greek words for nail and dissolution. In professional practice it is sometimes referred to informally as nail lifting, nail separation, or simply a lifted nail — though onycholysis is the correct clinical term and should be used when documenting nail conditions in client records.
Onycholysis is not a diagnosis in itself — it is a sign, meaning it is the visible result of an underlying cause. Identifying and addressing that cause is as important as managing the separation itself. In many cases the cause is mechanical and straightforward to resolve. In others, onycholysis is the presenting sign of a systemic or dermatological condition that requires medical assessment.
How It Looks and How to Recognise It
Onycholysis is usually immediately recognisable on an uncoated nail. The separated zone appears white or pale — sometimes slightly yellowish or opaque — because air has entered the space between the lifted plate and the exposed nail bed beneath. This distinguishes it from the healthy pink zone where the plate is still attached and the nail bed colour is visible through the plate.
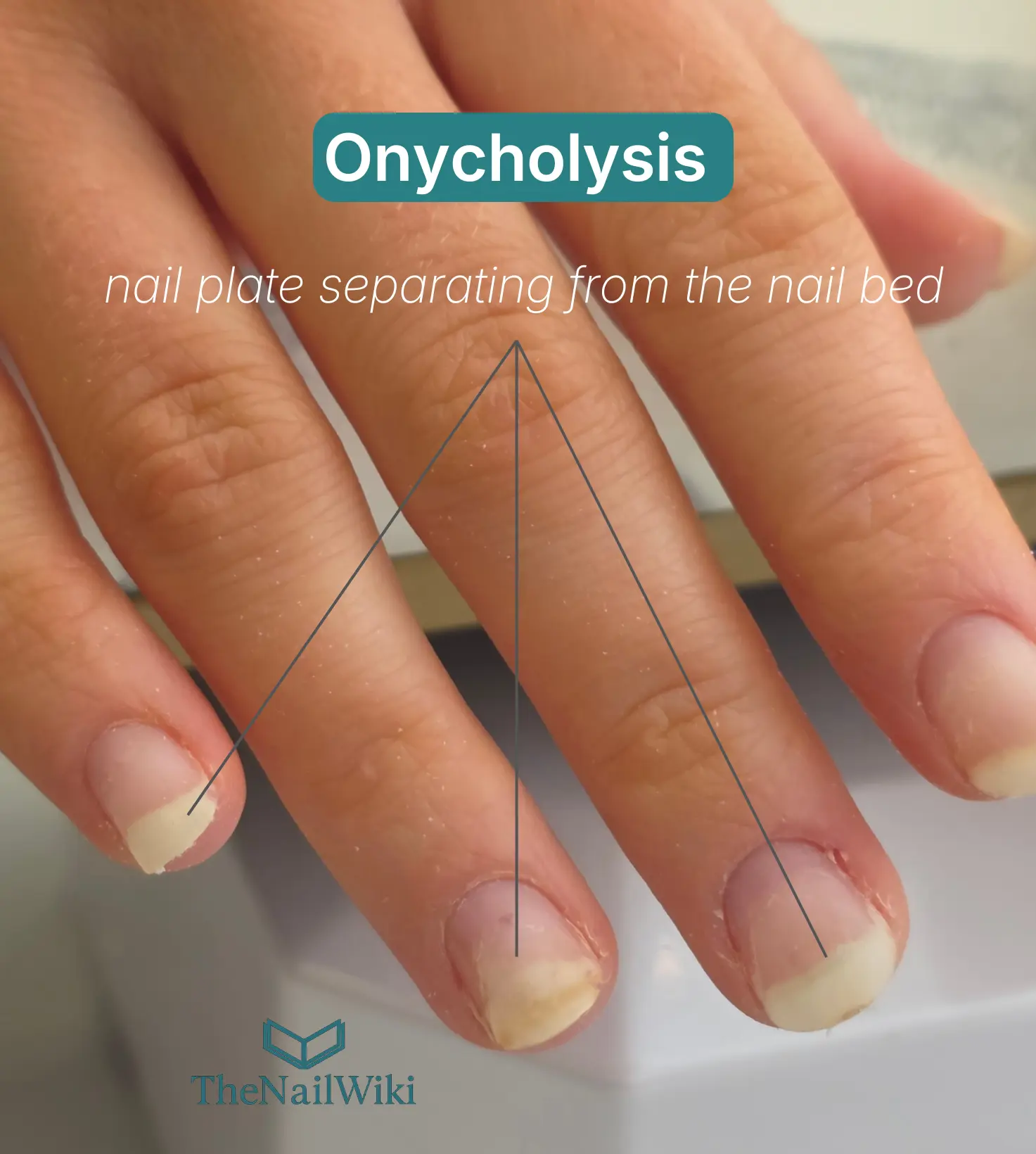
The separation almost always progresses from the free edge towards the base — distal to proximal in clinical terms. The boundary between the lifted and attached zones typically follows a curved or irregular line that mirrors the shape of the hyponychium. When seen from above, this line marks exactly where the nail bed ends its attachment to the advancing plate.
In mild cases, only a small area at the very tip is lifted. In more advanced cases, the separation may extend halfway or further up the nail. In severe or long-standing cases, secondary discolouration — yellow from debris, green from bacterial colonisation, or brown from trapped moisture — may be visible within the separation space.
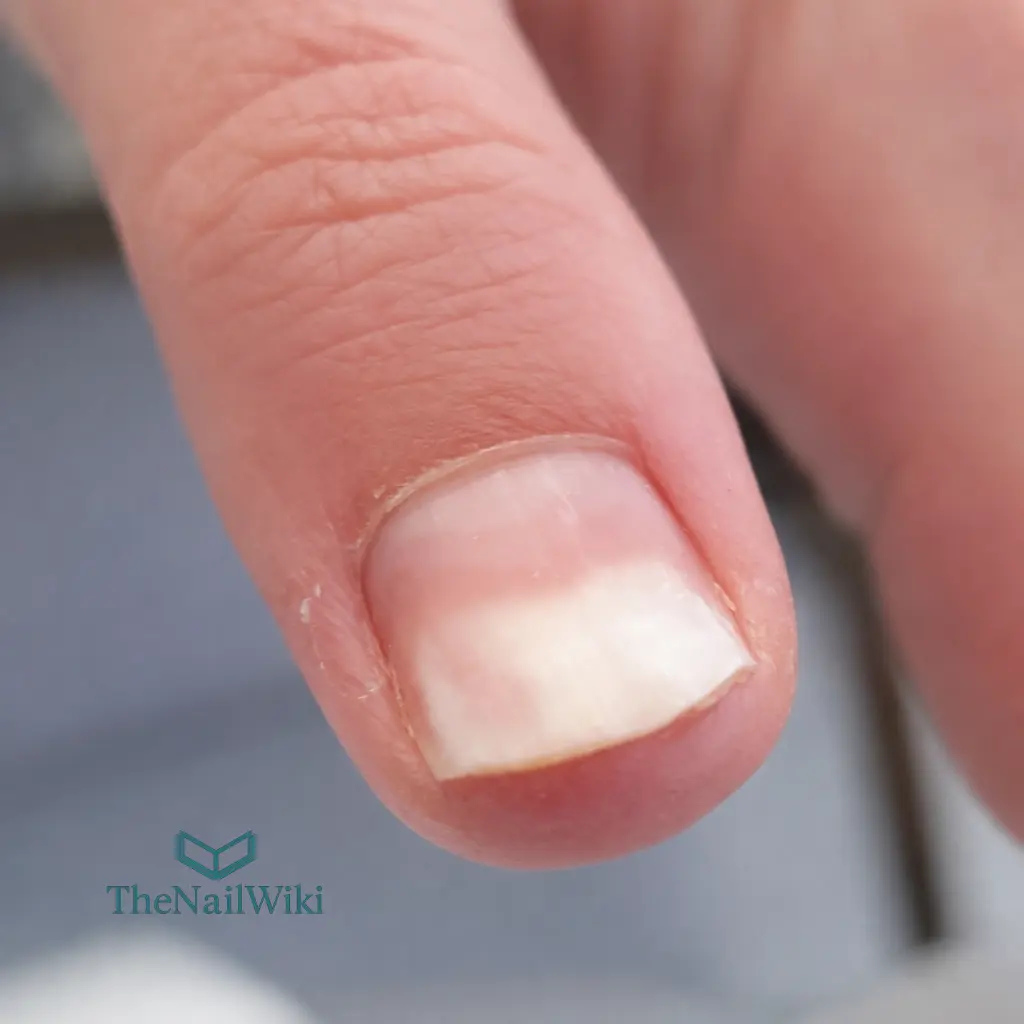
Under nail products: Onycholysis under a nail enhancement or gel polish is not always visible until the product is removed. A hollow sound when gently tapping a nail, or a client reporting sensitivity or discomfort at the free edge, may indicate a separation developing beneath the product. This is one reason product removal and careful nail bed assessment should be part of every appointment before reapplication.
Causes of Onycholysis
Onycholysis has a wide range of possible causes, which can be grouped broadly into mechanical, environmental, dermatological, and systemic categories.
Mechanical causes
- Direct trauma — catching, crushing, or impact to the nail tip
- Repetitive low-grade pressure — typing, playing instruments, or any activity that repeatedly stresses the free edge
- Long nails that flex excessively under pressure
- Aggressive cleaning beneath the free edge with a pointed tool
- Lifting nail enhancements left without removal, where the product mechanically levers the plate away from the bed
Environmental and chemical causes
- Prolonged or repeated immersion in water — softens the epidermal bond between plate and bed
- Regular contact with harsh detergents, cleaning products, or solvents
- Photo-onycholysis — separation triggered by UV light exposure in combination with photosensitising medications. The most common culprits are tetracycline antibiotics (particularly doxycycline), psoralens, and some fluoroquinolones. The client typically reports tender or painful separation of the fingernails following sun exposure whilst taking the medication
- Allergic reaction to nail products — contact sensitisation can cause the nail bed to react to product chemistry
Dermatological causes
- Psoriasis — one of the most common causes of onycholysis; psoriatic separation often has a characteristic red or pink border
- Onychomycosis — fungal infection advancing from the nail bed
- Lichen planus, contact dermatitis, and other inflammatory skin conditions
Systemic causes
- Thyroid disorders — both hyperthyroidism and hypothyroidism are associated with nail changes including onycholysis
- Anaemia and nutritional deficiencies
- Certain medications beyond tetracyclines — including some chemotherapy agents and oral retinoids
- Connective tissue disorders
Salon-Related Causes
In a nail salon context, the most frequently encountered causes of onycholysis are mechanical and product-related. Understanding these specifically helps professionals prevent recurrence and advise clients accurately.
Overfiling the nail plate. Filing the natural nail plate too aggressively — whether with a manual file or an e-file — thins the plate to the point where it can no longer maintain its bond with the nail bed. The case photographed above is a direct result of this. A thinned plate loses structural integrity and the plate-to-bed attachment progressively breaks down across the affected area.
Heat spike from the lamp during curing. Products that generate significant heat during UV or LED curing — particularly thicker gel layers or certain builder gels — can produce a heat spike intense enough to disrupt the plate-to-bed bond. Clients who report a sudden burning sensation during curing should not be dismissed. Repeated heat spikes at the same nail bed area can initiate or worsen separation.
Incorrect shape or apex placement. When a nail enhancement is built with an incorrect apex position or an unsuitable shape for the client’s natural nail — for example, a short almond where the growth point and stress area are left unsupported — the product distributes force unevenly during wear. Over time, this mechanical stress concentrates at the point of weakest attachment and can initiate or accelerate separation beneath the product.
Lifting enhancements not removed promptly. When a gel or acrylic enhancement lifts at the free edge and the client continues wearing it, the rigid lifting product acts as a lever — every time it catches or flexes, it applies force at the attachment boundary and progressively extends the separation beneath it. By the time the client returns for their next appointment, what began as a small lifting area may have advanced significantly into the nail bed zone.
Aggressive filing under the free edge. Some professionals file beneath the free edge to clean or prepare the nail. If this is performed too aggressively or too far back, it can disrupt the hyponychium — the seal at the junction of the free edge and fingertip — initiating a separation that then progresses.
Product contact sensitisation. In clients who have developed a sensitivity to nail product chemistry — particularly to acrylates in gel or acrylic systems — the nail bed may begin to react to the product above it, producing inflammation that breaks down the plate-to-bed bond. This type of onycholysis does not resolve until all contact with the sensitising product ceases. It is one of the reasons that patch testing and contact sensitisation awareness are important professional competencies. Read more: Contact Sensitisation and Nail Allergies →
Advising clients
Clients with onycholysis should be advised to keep nails short, avoid water immersion where possible, wear gloves for cleaning and dishwashing, and not attempt to clean beneath the lifted nail with any pointed instrument. Each of these actions can extend the separation further or introduce secondary infection into the space.
Professional Management
The professional management of onycholysis is straightforward but must be communicated clearly to the client, who may be hoping for a quicker fix than is possible.
- Trim back to solid attachment. Using nail nippers or scissors, trim the lifted nail plate back to the point where it is still firmly attached to the bed. Do not go further. Do not attempt to push the plate back down
- Do not apply product over the separation. Sealing the gap with gel, acrylic, or any other product traps moisture and debris against the exposed nail bed and significantly increases infection risk
- Keep it clean and dry. Advise the client to clean the exposed area gently, avoid prolonged water contact, and keep the nail short while recovery progresses
- Identify and address the cause. Without resolving the underlying cause, the separation is likely to continue or recur. Go through the likely causes with the client — trauma history, moisture exposure, products used, any skin conditions — and address what can be changed
- Document it. Record the condition in the client’s nail consultation notes, including its extent, likely cause, and the advice given. This protects both the client and the professional
Traditional remedies used by nail professionals
Across Eastern Europe, nail professionals have long used Monarda oil (also known as wild bergamot or bee balm oil) for clients experiencing nail separation and bacterial discolouration. It is widely used within the professional community and many technicians and their clients report positive results. The oil contains active compounds — primarily thymol and carvacrol — which have demonstrated antimicrobial and antifungal properties in laboratory studies, including activity against organisms that commonly colonise the lifted nail space. This gives the traditional use a plausible biological basis. It is important to understand, however, that Monarda oil cannot reattach the nail plate — onycholysis is mechanical separation and no oil or product can reverse that. Its value is in helping to control microbial colonisation in the lifted space while the nail grows out. This is a traditional professional remedy rather than a medical treatment — if you are dealing with an active infection or have any health concerns, seek medical advice.
Purchase Monarda Oil on Amazon →
Affiliate link — TheNailWiki may earn a small commission if you purchase through this link, at no extra cost to you. This does not influence the information on this page.
Onycholysis and the Green Nail
When onycholysis is present — whether beneath a nail product or on a natural nail — the warm, moist space between the lifted plate and the exposed nail bed creates ideal conditions for bacterial colonisation. The most common organism to colonise this environment is Pseudomonas aeruginosa, a gram-negative bacterium widely present in the environment. As it metabolises in this space, it produces a green-blue pigment called pyocyanin, which stains the nail bed and the underside of the plate.
This green discolouration is frequently — and incorrectly — referred to as a mould infection. It is not mould. It is a bacterial colonisation. This distinction matters because the management is entirely different: fungal nail infection requires antifungal treatment; Pseudomonas is a bacterium and antifungal treatments have no effect on it whatsoever. A Pseudomonas bacterial stain resolves with a clean, dry environment as the nail grows out — and where medical treatment is needed, it requires antibacterial treatment, not antifungal. Read the full guide: Green Nail Syndrome →
Professional response to a green nail
Remove all product. Trim the nail plate back to solid attachment. Advise the client to keep the area clean and dry. No new product should be applied until the green discolouration has completely grown out — which may take several months depending on how far up the nail it extends.
If the green area is extensive, if there is pain, swelling, or pus, or if the client has any health conditions affecting immunity, refer for medical assessment. A Pseudomonas infection that progresses beyond a surface stain into active infection requires medical treatment.
For a complete guide to green nail syndrome — including causes, recognition, misconceptions, and full management protocol — read: Green Nail Syndrome (Nail Greenies) →
When to Refer
Not all onycholysis requires medical referral — but some does. The following presentations should always prompt a recommendation to seek medical assessment:
- Onycholysis with no identifiable mechanical or environmental cause
- Separation beginning at the base or sides of the nail rather than the free edge
- Rapid or progressive separation
- Multiple nails affected simultaneously without a clear shared cause
- Presence of pain, swelling, redness, or pus around the nail
- Associated skin changes on the fingers or elsewhere on the body
- Secondary discolouration that does not resolve as the nail grows out
- Any dark or pigmented streaking within the separation zone
- A new pigmented band, pigment spreading onto the surrounding skin (Hutchinson sign), a visible mass, ulceration, or bleeding from a single nail — these are potential signs of a nail unit tumour and require urgent dermatology assessment, not monitoring
- The client has diabetes, peripheral vascular disease, immunosuppression, or any condition that significantly affects healing — the stakes are higher and earlier medical involvement is warranted
Recovery and Timeline
Once the cause has been resolved and the lifted section trimmed back, the nail bed will begin to re-establish its attachment to the advancing plate as it grows forward. The recovery timeline depends on how far the separation extended and the individual’s nail growth rate.
Recovery timeline reference
- Fingernails grow approximately 3.0 – 3.5 mm per month
- A separation extending halfway up the nail may take 3 or more months to fully resolve
- Full nail regrowth from matrix to free edge takes approximately 6 months
- Toenail recovery is significantly longer — up to 12 – 18 months for full regrowth
It is important to set this expectation with clients clearly from the first appointment where the condition is identified. Many clients expect the nail to look normal within a few weeks. Understanding that recovery is measured in months — and is dependent on the cause being fully resolved — prevents frustration and maintains trust throughout the recovery period.
Common Misconceptions
❌ “Applying product over lifted nail will hold it in place”
Sealing over onycholysis does not re-attach the plate — it creates a sealed, warm, moist space where bacteria and fungi can thrive. The separation will continue beneath the product, often undetected, until the product is removed. This is one of the most harmful practices a nail professional can perform on a client with onycholysis.
❌ “The green colour means it is mould”
The green colour associated with lifted nail products is caused by Pseudomonas aeruginosa bacteria, not mould. The distinction matters for correct management and for accurate client communication. Telling a client they have mould is both incorrect and unnecessarily alarming.
❌ “Onycholysis is always caused by nail products”
Products can cause or contribute to onycholysis, but they are far from the only cause. Psoriasis, thyroid conditions, trauma, moisture, fungal infection, and medication are all common causes. Assuming a nail product is always responsible delays identification of the true cause and may mean a client does not receive the appropriate medical assessment they need.
❌ “Pushing the plate back down will re-attach it”
The plate-to-bed bond cannot be mechanically re-established. It must re-form biologically as new plate grows forward over a recovering nail bed. Pressing a lifted plate down achieves nothing and risks introducing debris or bacteria into the separation space.
Frequently Asked Questions
What does onycholysis look like?
Onycholysis appears as a white, pale, or opaque area beginning at or near the free edge of the nail. The colour change is caused by air filling the space between the lifted plate and the nail bed beneath. In advanced cases, additional discolouration — yellow, green, or brown — may appear within the separation space due to debris accumulation or secondary bacterial colonisation.
Can onycholysis heal on its own?
The separated zone will not re-attach spontaneously — but once the cause is resolved and the lifted section is trimmed back, the nail bed will form a new attachment to the advancing plate as it grows forward. Recovery is possible in most mechanical and environmental cases provided the cause is genuinely removed.
Is onycholysis painful?
Onycholysis itself is typically painless — the separation occurs gradually and the nail plate has no nerve supply. However, the exposed nail bed is sensitive, and if the lifted area catches on clothing or objects it can be uncomfortable. If there is significant pain, this may indicate a secondary infection or an underlying condition and warrants medical assessment.
Can I have nail enhancements with onycholysis?
No. Product should not be applied over an area of onycholysis. The separation must be trimmed back to solid attachment first. Product can be applied to the remaining attached nail, but the separated zone must be left bare until the attachment has re-established as new plate grows forward.
How long does onycholysis take to resolve?
Recovery time depends on the extent of the separation and the client’s nail growth rate. Fingernails grow approximately 3 to 3.5 mm per month. A separation extending halfway up the nail may take three or more months to fully resolve after the cause has been addressed. Toenail recovery takes significantly longer — up to twelve to eighteen months.
Related Library Pages
Nail Anatomy
Nail Conditions
Professional Safety
Some linked pages are currently in development and will be published progressively.
Professional Disclaimer
The information on this page is provided for educational purposes and is intended to support the professional knowledge of nail technicians and nail educators. It does not constitute medical advice. Any client presenting with onycholysis without a clear identifiable cause, or with additional nail or skin changes, should be advised to seek assessment from a qualified medical professional.
About the Author
Radina Ignatova
Professional Nail Expert since 2014 | International Nail Educator | Founder of TheNailWiki and Artistic Touch Nail Training Academy
Radina Ignatova is a Professional Nail Expert since 2014 and an International Nail Educator specialising in dual forms, gel systems, polygel application, advanced nail structure, E-File techniques and professional salon safety.
She founded TheNailWiki to provide clear, safety-led nail education accessible to everyone, and Artistic Touch Nail Training Academy to deliver structured professional online nail courses.
Her teaching philosophy is centred on honest education — demonstrating real salon challenges, practical corrections and performance-based techniques rather than presenting only polished results.
Based in Scotland, UK, Radina contributes to advancing professional standards within the nail industry through structured educational resources and technical training.
Read full bio →About TheNailWiki
TheNailWiki is an independent educational platform dedicated to providing accurate, safety-led and professionally informed nail care information to professionals and enthusiasts worldwide. All content is created by qualified nail industry professionals and reviewed for technical accuracy.
Our mission is to provide accurate, safety-focused and professionally informed nail education that is accessible to everyone. For structured professional training, advanced masterclasses, and specialist technique courses, visit Artistic Touch Nail Training Academy.
This library page is published by TheNailWiki — an independent nail education resource maintained by nail industry professionals. Content is safety-led and professionally informed.
